United pregnancy has the worst maternal mortality index in developed countries;60% of them are preventable.Lauren Bloomstein's death - in the same hospital where he worked as a neonatal nurse - illustrates deep disparity: the health system focuses on babies but often ignores their mothers.Sponsors: By :: Univision, Sep 29, 2017 - 02:30 PM EDTComparte
As a neonatal intensive care nurse, Lauren Bloomstein had taken care of other people's babies for years.Finally, at 33, he expected his.The idea of becoming a mother had her beautifies. “Nunca antes la había visto tan feliz y tan vivaz”, recuerda su esposo, Larry.
When Lauren was 13 years old, his mother died of a heart attack.She lived with her older brother for a while and then with a neighbor in Hazlet (New Jersey), who was like a substitute mother, but in many ways she had to grow alone.The opportunity to create her own family, to be the mother she never had, she touched deeply."Everything he always wanted was to be loved," said Frankie Hedges, who welcomed her during her adolescence, considering her as a daughter."I think everyone loved her, but nobody in the way she wanted to be loved".
Read This Story in English
Más allá de las náuseas del primer trimestre, Lauren no tuvo problemas o molestias durante el embarazo.She felt "tired at the beginning and sore at the end," says Jackie Ennis, her best friend from high school, with whom she spoke at least once a day.“The weight it owed increased, Lucia fabulosa.He felt good, worked as much as he could ”(at least three shifts of 12 hours a week until his ninth month of pregnancy).Larry, who is a doctor, helped her monitor her blood pressure at home, and everything was normal.
Relacionados
¿Conoces a alguna mujer que haya muerto o haya estado cerca de morir durante el parto? Ayúdanos a investigar la mortalidad materna
In his free days, he organized for the arrival of the baby, choosing strollers and baby seats for car, and supplying clothes and diapers.After a last vacation before the baby in the Caribbean, she and Larry bought the house of their dreams: colonial bricks with black countervanas and a large garden in Moorestown, not far from Larry's new work as an orthopedic surgeon in Camdem.Lauren wanted the baby's sex to be a surprise, so when he decorated the room, he did not paint the walls (he assumed that he would have a lot of time to choose colors later).
Although I knew there were things that could go wrong, I was not worried: I felt the normal anxiety experienced by future mothers. His only anguish was having a premature birth.“You have to stay there inside at least 32 weeks.I know the problems that babies face before week 32.So don't go out too early, ”he told his baby.
When he arrived at 39 weeks and six days, on Friday, September 30, 2011, she and Larry led the Monmouth Medical Center in Long Branch, the hospital where both met in 2004 and where much of Lauren's professional career had elapsed.He thought that if someone would take care of her and her baby, they would be the doctors and nurses with whom she worked daily.It was especially close to his obstetrician/gynecologist, who had been resident in Monmouth at the same time as Larry.
Although he had no contractions, Lauren and his doctor agreed to induce childbirth.He was on duty that weekend and was sure to be able to personally take care of the birth.
Induced deliveries are usually slow and Lauren's lasted until the next day.Her friend Ennis spoke with her on the phone several times. “Dijo que se sentía bien, que simplemente estaba muy incómoda”.At one point, Lauren felt a sudden and sharp back pain, near her kidneys or liver, but nurses increased her epidural and the stab.
Inductions have been associated with high caesarean section, but Lauren progressed well enough to have a vaginal delivery. El sábado 1 de octubre a las 6:49 pm, 23 horas después de ingresar en el hospital, Hailey Anne Bloomstein nació.He weighed 2.32 kilos.Members of their families had camped in the waiting room and now they went to the delivery room and marveled to see how Lauren seemed to shine.
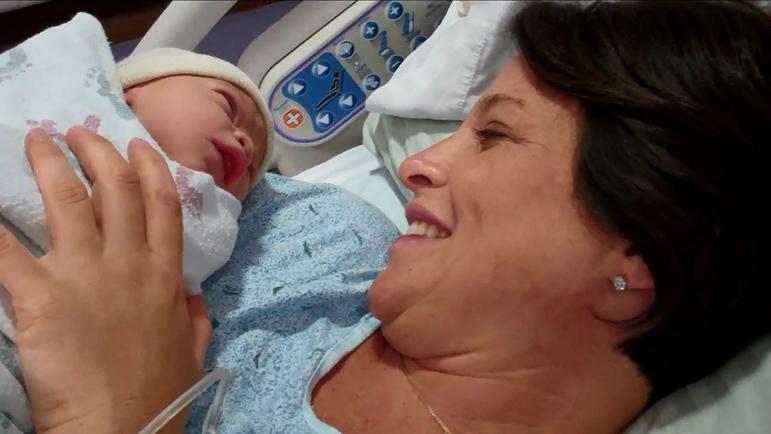
Larry floated in his own euphoria cloud, taking photos with his phone.In a 35 -second video, Lauren holds her daughter about her chest, stroking her face.Hailey is wrapped in the hospital pastel sabanitas, unusually alert for a newborn;She studies her mother's face as if she tried to decipher a mystery that will never be resolved.The nurses and the rest of the team of the delivery room come and go in the background in that form of those who believe that everything has elapsed exactly how it should be.
At that time Lauren looks directly at the camera, with his overflowers.
20 hours later I was dead.
Cargando Video...Esta mujer falleció 20 horas después de dar a luz a su bebécada año en Estados Unidos entre 700 y 900 mujeres mueren durante el embarazo por causas relacionadas con el parto, y 65,000 presentan complicaciones que las acercan a la muerteAmerican women are three times more likely to die than Canadians during the maternal period (defined by the centers for the control and prevention of diseases and from the beginning of pregnancy to a year after childbirth or abortion), and six times more timesthan the Scandinavians.
In the rest of the developed countries and many others less industrialized, maternal mortality rates have been reduced;The British medical magazine The Lancet recently reported that the index has dropped so dramatically that "a man has more chances of dying while his couple is pregnant than herself".But in the United States, maternity deaths rose between 2000 and 2014.In a recent analysis of the CDC Foundation, almost 60% of those deaths were preventable.
Aunque la mortalidad materna es significativamente más común en las afroamericanas, las mujeres de bajos recursos o que viven en zonas rurales, las complicaciones del embarazo y parto matan a mujeres de cualquier raza o etnia, nivel educativo o socioeconómico por igual, en todo Estados Unidos.
Propublic and NPR spent the last months investigating social networks and other sources, and finally identified 450 pregnant women and new mothers who died since 2011.The list includes teachers, insurance runners, journalists, a spokeswoman for Yellowstone National Park, a co-founder of the YouTube channel Whatsupmoms, and more than a dozen doctors and nurses like Lauren Bloomstein.
They died of cardiomyopathy and other heart problems, massive hemorrhages, blood clots, pregnancy -induced infections and hypertension (preeclampsia), as well as strange causes.Many died days or weeks after leaving the hospital.Maternal mortality has become so common that three mothers who died, including Lauren, were treated by the same obstetrician.
The reasons for these high indices in the United States are varied.The new mothers are greater than they used to be, with more complex medical stories.Half of pregnancies in the United States are not planned, so women do not address their health problems in advance.The highest prevalence of caesarean sections entails more complications that can be mortal.The fragmented health system hinders mothers, especially those without access to health insurance, to obtain the attention they need.The confusion about how to recognize alarming symptoms and how to treat obstetric emergencies makes health providers more likely to make mistakes.
However, the worsening of maternal mortality rates contrasts pronounced with great progress in saving babies' lives.Infant mortality has been reduced to its lowest point in history, CDC reports, which reflects 50 years of public health efforts to prevent congenital defects, reduce premature childbirth and improve the possibility of life for very premature babies.The number of children who dies annually in the United States (about 23,000 in 2014), exceeds that of mothers who die, but the proportion has been reducing.
The dissonance between the statistics of mothers and children underlines an issue that has constantly emerged in the reports of Propublic and NPR. En décadas recientes, bajo la presunción de que se ha superado la mortalidad materna, el sistema médico estadounidense se ha enfocado más en la seguridad y supervivencia del feto y del infante que en la salud y el bienestar de la madre.
"We care very much about the vulnerable and small babies," says Bárbara Levy, vice president of health and public policies of the American Congress of Obstetricians and Gynecologists.Health Care.Meanwhile, "we do not pay enough attention to those things that can be catastrophic for women".
In the Network of Maternal-Fetal Medicine Units funded by federal funds, the preemineof infants' lives (the rest, attend to both).Under Title V, a federal program that supports the health of mothers and babies in the country, in 2016 6% of subsidies to mothers programs were allocated, which contrasts with 78% destined for infants and children with special needs.
The notion that babies deserve more care than mothers are also rooted in Medicaid programs, which pays for 45% of births.In many states, the program includes the mother for 60 days during the postpartum, while babies are given coverage for a full year.
En cuanto a los proveedores de servicios médicos, los avances tecnológicos han aumentado la diferencia entre los cuidados a las madres y los cuidados a los fetos y bebés."People were excited about the ability to make ultrasound, then ultrasounds in high definition and other invasive procedures, such as the use of needles in the amniotic cavity," said William Callaghan, head of the Maternal Child section of the CDC.
The growth of maternal-feetal medicine has focused so much on the fetus that in 2012 the young doctors who wanted to work in that area did not have to spend time learning to take care of mothers who give birth."The training varies depending on the US area," says Mary D’Alton, director of Ob-Gyn, at the Medical Center of Columbia University, and author of articles about disparity in the care of mothers and babies."There were some students who even finished their maternal-fetal medicine training without having been in a childbirth room.".
In the last decade, at least 20 hospitals have established multidisciplinary fetal care centers for babies with different high -risk problems.For now, just a hospital in the United States - New York Presbyterian/Columbia - has a similar program for high -risk pregnant women.
En las unidades tradicionales de maternidad, también los bebés son monitoreados más de cerca que las madres durante y después del parto, dijeron activistas a favor de la salud materna a ProPublica y NPR.Newborns in the minimum risk are taken to an intensive care unit such as that in which Lauren Bloomstein worked, to be monitored by a trained personnel for the worst.Meanwhile, their mothers are treated by nurses and doctors who expect things to march well and are not prepared when they stop being.
Cuando las mujeres son dadas de alta, reciben información de forma rutinaria sobre cómo dar pecho y qué hacer si el recién nacido se enferma, pero no necesariamente son entrenadas para distinguir si ellas necesitan atención médica. “Fue solo cuando tuve mi propio bebé que me di cuenta: ‘Dios mío, era información insuficiente’”, explica Elizabeth Howell, profesora de obstetricia y ginecología en la escuela de medicina del Hospital Mount Sinai de Nueva York.“Because of the way we were trained, we did not give enough information to women about how to handle their postpartum health.The focus is always on the baby and not in them ".
In 2009, the Joint Commission, which accredits 21,000 health establishments in the country, adopted a series of perinatal “basic measures”, national standards that have shown to reduce complications and improve results for the patient.Four of the measures are aimed at the baby's health.One (lower the caesarean section) is focused on mother's health.
Meanwhile, life measures that have been widely accepted in other developed countries, and in a few states such as California, are not yet assumed in the United States hospitals.For example, preeclampsia, high blood pressure that occurs only during pregnancy or postpartum and that can trigger strokes and spills, kills five women per hour in the world.But in developed countries, it is very treatable.The key is to act quickly.
Standardizing its approach, Great Britain has reduced deaths for this cause to one million, a total of two deaths between 2012 and 2014.On the contrary, in the United States, preeclampsia still represents 8% of maternal deaths (50 to 70 women per year).Including Lauren Bloomstein.
serie de libros"You got to be kidding.Acéptala, it would be fabulous, ”insisted Frankie Hedges.
Lauren gave up and the editor gave him the role of the older sister, Meg.He appeared on the cover of four books, such as the typical nineteenth century with his long brown hair and a pearl necklace.The determined expression of his face was all Lauren."I didn't want compassion, or wanted mercy," explains Jackie Ennis."He didn't talk much about his feelings about his mother.I saw it as if it was his problem and was going to do everything in his possession to become someone productive ”.
During high school, Lauren decided that he would become a nurse and chose a two -year program at the Brookdale Community College.She worked at a doctor's office to earn money to pay for the registration and lived in an apartment in the garage that Hedges and her husband had adapted especially for her, who often took care of her twins.
Lauren "was not a very affectionate person," says Hedges.But he did appreciate being part of a family again."You can't believe how happy it is," said Ennis once to Hedges."We left and said that: 'I have to go home for dinner!".
After graduating in 2002, Lauren was assigned to the Monmouth Medical Center, a complex a few minutes from the great framework that is the RWJBARNAS HealthSystem health system, affiliated with the University of Drexel School of Medicine, Philadelphia.
His first work was in the surgery unit, where his clinical and ethical work skills were recognized. “No puedo recordar a muchos trabajadores a quienes respetara tanto como a Lauren”, escribió Diane Stanaway, directora clínica de enfermería del Monmouth, en un tributo profesional en 2005: “¡Qué joven y enfermera tan activa!”.Larry remembers that when a senior hospital executive needed to operate, he gave Lauren's greatest flattering when he chose her as one of her two exclusive nurses.
Larry Bloomstein, who began working in that same unit as a resident of orthopedic surgery in 2004, was dazzled.He liked his independence. “No sentía la necesidad de apoyarse en nadie más para nada”.Even when trying to resurrect a patient through the CPR, he kept calm, says Larry.
He thought that the difficulties she faced in childhood gave her "self -confidence.He was not worried about small things ".After meeting Larry, Lauren told Ennis: “I met this boy.He is a doctor and is very friendly ".The first appointment was a Bruce Springsteen concert.Five years later they married Long Beach Island, on the coast of Jersey.One of Lauren's favorite books was The Catcher in the Rye."He identified with Holden Caulfield, a character who rescued children," says Larry.
When an opportunity was opened to work in the prestigious Neonatal Care Unit of Monmouth in 2006, she did not hesitate to postulate.
The hospital has the fifth most busy maternal care unit in the state.In 2016, 5,449 babies were born there. Monmouth fue calificado como un hospital de nivel “A” por Leapfrog, una organización que promueve la seguridad en la atención médica, y cumplió con todos los estándares de seguridad en las unidades de maternidad, como índices de cesáreas y partos electivos inducidos, dijo una vocera de la entidad.Its intensive care unit, a level III ease for high -risk newborns, is the oldest in New Jersey.
"Not everyone can work in a neonatal intensive care unit.Babies are small and many people are not accustomed to seeing so tiny babies, ”explains Katy Di Bernardo, a veteran nurse who has been working in the unit for 20 years.
There work nurses, neonatologists, specialists in respiratory therapy and residents.According to Di Bernardo, Lauren, he fit instantly.
One of the things that Lauren of his work most worshiped were the links he did with the families of the babies.Nurses took care of the same newborns throughout their stay, sometimes for weeks or months. Era muy buena con los padres, muy buena para “calmar a la gente con mucha ansiedad”, cuenta Larry.Frequent.
I also appreciated the great friendships that a place like a Nicu can forge.The neonatal care floor was almost a world in itself.Lauren Byron, another long -standing nurse in the place illustrates it: “There is a lot of stress and pressure and you are in life or death situations.You develop very close relationships with some people ".The environment tends to attract strong personalities.In the Bloomstein Family Football Power, Lauren had the nickname of "The Fighter", so he immediately fit.But he could defend himself without hurting others."It was one of those people who please everyone," said Byron.
"She was very friend of my wife and felt very comfortable with me," Vaclavik said during her testimony in court, in 2015.
Luego de terminar su residencia, Vaclavik comenzó a trabajar para Ocean Obstetric & Gynecologic Associates, una próspera clínica que incluía a muchos profesionales médicos entre sus clientes.Vaclavik favored natural birth, part of a movement that seeks to reduce the number of caesarean sections that tend to have a slower recovery and greater complications than a vaginal birth.While in the state the caesarean section was 37%, that of the Monmouth Hospital was 21% for 2016.
Neonatal nurses had many opportunities to observe Vaclavik and other obstetricians in action (someone from the neonatal care unit should always be in each birth that showed indications of complications, as well as in each caesarean section)."We always joked: they call us even for the cuticle of a nail," Dibernardo said.
Lauren was so impressed by Vaclavik that he not only chose him as his doctor, but he recommended it to his best friend."She said: you have to see you with this guy.He is a good doctor.Good doctor, ”said Ennis.
But in other things, Nicu and childbirth team were very remote.Neonatal nurses focused on their fragile patients (that satisfaction of when they returned healthy home and pain when that did not happen).Once Ennis asked Lauren how he dealt with the babies who did not survive."It must be terrible," he said.Lauren replied: "Yes, but we save more than we lose".
The deaths were less and less frequent during childbirth and when a mother faced complications that endanger her life, the news did not always reach Nicu.This happened when Tara Hansen, a special education teacher who was 29 years old, died from an infection after giving birth to her first child in March 2011.Lauren, who was three months pregnant, did not find out about the news.
Hansen lived in Freehold, New Jersey, with her husband Ryan, her boyfriend from school.His pregnancy, like Lauren, had no complications, and gave birth to a healthy 4 kilos baby.But Hansen suffered a heartbreaking in the vagina during childbirth.He had signs of infection and was also discharged, which would lead her husband to sue the clinic later.
Hansen was admitted again in Monmouth with what legal demand would then catalog as "severe pain, which could not be tolerated by any human being".The diagnosis was necrotizing fasciitis, better known as the ‘Comment Bacteria’.Two days later, Hansen was dead.
More about pregnancy
SALUDThe increase in moisture due to climate change causes increased suicides, according to research
4 min de lecturaSALUDMas Premature delivery risk: The dangerous effects of climate change in pregnancy
1 min de lecturaSALUDStudy of more than two decades determines that Tylenol (acetaminophen) can be risky for pregnant women
4 min de lecturaSALUDHe did not get pregnant and lost his baby by getting sick from Covid-19
2 min de lecturaOne of Vaclavik's colleagues had been in charge of childbirth.Vaclavik himself was the one who discharged him.According to court documents, he claimed that the nurses had not informed him of Hansen's symptoms and that if he had known that the vital signs were not stable, he would not have registered.In the end, the hospital and nurses eventually signed an agreement for 1.5 million dollars.
The demand against Vaclavik and his colleagues is still pending.
Vaclavik did not respond to several applications for Propublic and NPR interview, including an email containing the list of questions.His lawyer replied: “In view of the fact that this matter is litigating, the dr.Vaclavik respectfully declines to comment ”.
Alleging as a reason the privacy of the patients, the spokeswoman of Monmouth, Elizabeth Brennian also refused to discuss the specific case."We are very sad about the pain that these families have experienced for their loss," he said in a statement.
El primer presentimiento que tuvo Larry BloomsteinLarry had been with Lauren during the last 24 hours.Aware that he was a husband and not doctor, he tried not to intervene too much.Now, however, he pressed Vaclavik: What happened to his wife?He “told me:‘ This is frequent.We do many abdomen surgeries.It is definitely reflux, ”he said.According to Lauren's history, the obstetrician prescribed an antacid named Bicitra and an analgesic opioid called Dilaudid.Lauren vomited them.
His pain was 10 on a 10 scale, he told Larry and nurses. Las enfermeras anotaron: “La paciente no logra quedarse tranquila”.Just as worrying was the reading of his blood pressure that he was rising.An hour after delivery, he was in 160/95, and 60 minutes later he had climbed at 169/108.During his last prenatal consultation, Lauren had tension at 118/69.Larry was not a specialist in the Obstetrics area, but he knew enough to ask the nurses: could it be preeclampsia?
Preeclampsia, or pregnancy -related hypertension is a condition that affects between 3% and 5% of pregnant women in the United States: up to 200,000 women per year.It can give anyone and arise from nowhere, although the risk is greater for African -American, women with pre -existing conditions such as obesity, diabetes or kidney problems and mothers over 40 years old.It is more common during the second half of pregnancy, but it can develop in the days or weeks after childbirth and may arise suddenly and dangerously.
In view of the fact that the typical treatment for preeclampsia is to give birth as soon as.
Como Larry sospechó, la presión arterial de Lauren estaba más allá del límite.What I did not know was that it had been like this since she entered the hospital (147/99, according to admission documents).During childbirth, he had 21 systemic readings at or above 140 and 13 diastolic readings at or above 90, indicates his medical history.For eight hours its blood pressure was not monitored, the New Jersey Health Department concluded later.In that same time period, the baby's vital signs were constantly monitored, Larry clarified.
In its deposition, Vaclavik described the reading of 147/99 as "high" compared to the usual Lauren readings, but did not catalog it as abnormal.I would have "used as parameter 180/110" to suspect preeclampsia, he said.Even so, he acknowledged that with this blood pressure, "I could recommend more frequently monitor Lauren, in retrospect".
Prominent medical organizations in the United States and the United Kingdom have a different point of view. Recomiendan que cualquier aumento por encima de 140/90 para mujeres embarazadas sin historia de hipertensión sea considerado como preeclampsia.When systolic reading reaches 160, it is suggested that an anti-hypertensive and magnesium sulfate treatment will begin "as soon as possible" to prevent attacks, according to the guidelines of the Alliance for Innovation in Maternal Health.When there are other symptoms such as upper abdominal pain, the situation is considered even more urgent.
This basic approach is not new: a text widely used and published in 1997 and entitled ‘Essential curriculum for maternal and newborn health’, dictates the same.Even so, the failures in the diagnosis of preeclampsia or in differentiating it from other chronic hypertension problems persist.
California researchers who studied deaths due to preeclampsia for several years found something amazing: “Despite the triggers who indicated a severe deterioration in the patient's condition, health providers did not detect or respond to these signs, which led to delays in the diagnosis and treatment".
Preeclampsia symptoms (inflammation and rapid weight gain, gastric pains, vomiting, headache and anxiety) are often confused by the typical pregnancy or childbirth aches."We do not have a proof of itself or not for it," says Eleni Tsigas, executive director of the preeclampsia foundation."Many doctors do not necessarily see it frequently".Outdated notions, such as that giving birth to heals the condition, or little familiarity on how to proceed and lack of preparation before the crisis can further affect the response capacity.
The fact that Lauren gave birth for a weekend could also have played against him.Hospitals have different teams during weekends, which makes the challenges even greater when it comes to a crisis.An analysis of the Baylor Medicine School, from 45 million pregnancies in the US between 2004 and 2014, found that moms that give birth to a Saturday or Sunday have 50% higher mortality rates, as well as more blood transfusions andperineal tearing.The "weekend" effect is also associated with higher featality indices in heart attacks, spills and cerebral trauma.
According to Lauren's records, Vaclavik did order a laboratory exam for preeclampsia at 8:40 pm, but a nurse scored half an hour after there was no abnormal laboratory tests.(According to Larry, the results were just at the limit).Larry began to press to call a specialist.Vaclavik attributed Lauren's pain to an inflammation of the esophagus, which had happened before, he said in his statement.
At 10:00 pm, according to Lauren's medical history, he called the gastroenterologist who asked for an X -rays and other tests, as well as more Dilaudid and antacids such as Maalox and Protonix.None relieved it.
Meanwhile, Larry decided to call his colleagues from the Trauma Unit of Cooper University of Camden.During his training, the most important lesson he had learned was to ask for help: "If there is a problem, I immediately involve another doctor".Luckily, the doctor who on duty was a woman who had just become a mother."You can stop talking. Sé lo que es”, le dijo e indicó que Lauren tenía el síndrome de HELLP, un acrónimo para la peor versión de preeclampsia, que se caracteriza por la ruptura de glóbulos rojos, elevado nivel de enzimas del hígado y bajo conteo de plaquetas, una deficiencia de coagulación que puede generar exceso de sangramiento y un ACV hemorrágico.
Harry's colleague urged him to stop wasting time.The high lauren pressure, vomiting and pain in the area of their kidneys were symptoms of rapid deterioration. “Tu esposa está en peligro”, le dijo la doctora especialista en trauma (quien no respondió a la solicitud de comentarios que le hicieron ProPublica y NPR).
análisis"It's never one thing," says Roberta Gold, a member of the Patient Security Council in female care care, whose daughter and grandson died in 2010 due to a blood clot during pregnancy."It is always a waterfall or combination of things.It's like a slow -chamber derailment ".
The last 16 hours in Lauren's life are consistent with that nefarious pattern.Concerned about what the doctor specializing in trauma told her, Larry immediately turned to Lauren doctors.But they insisted that the exams did not show preeclampsia.Shortly after, Larry's colleague called to monitor Lauren's condition."I don't believe in those laboratory exams.They should not be wise.I'm sure my diagnosis.Repeat them, ”he said.
Meanwhile, Lauren's agony was unbearable.Now she felt too much pressure on the voltage measurement that wrapped her arm, so at 10:30 pm the nurse decided to take it out."We know that blood pressure is high, it makes no sense to take it again," he said.According to Lauren's medical history, his blood pressure was without monitoring for an hour and 44 minutes.
Larry had given up calling a specialist who could come to the hospital so late on a Saturday, but convinced Vaclavik to call a general surgery resident.At 11:55 pm, according to nurses, Lauren begged: "Do anything to stop this pain".Vaclavik prescribed morphine, which had no greater effect.
Shortly after midnight, his blood pressure reached 197-117 and Lauren began to complain about headache.While Larry saw his wife's face, he realized that something had changed."Suddenly he looked calm and calm, as if he were trying to fall asleep.".He gave Larry a little smile, but only the right part of his mouth moved.
In an instant, Larry panicked.Asked Lauren to raise his hands.Only his right arm reacted.He lifted the sheets and pinch him on his foot, to test Babinski's reflection (in a normal adult the big toe automatically moves down).Lauren's right finger moved as he should.But his big toe of the left foot does not.While Larry examined her, Lauren realized what was happening to her.“He looked at me and said:‘ I'm afraid, I love you ’.I'm sure at that time he understood everything.He realized that ... he was not going to survive ".
A brain scanner confirmed the worst: the ascending blood pressure unleashed a cerebral hemorrhage.These brain attacks tend to be more mortal than those caused by blood clots.Surgeons sometimes manage to save the patient's life, but only if they act quickly.
Larry was realistic: I knew that even the best stage would be devastating.Surely Lauren would be totally or partially paralyzed.It would never be the mother who dreamed of being.I would never be a nurse again.But at least I had a chance to survive.When the neurologist arrived, Larry asked him if there was hope.The doctor replied: "That's why I'm here, there is hope".
Larry began to congregate the relatives to Lauren, his parents, his brother, Frankie Hedges and her husband Billy, Jackie Ennis.On the phone he tried to lessen the severity of the stage, but everyone imagined.When Larry's mother arrived, the hospital entrance was closed and Larry and Vaclavik went out to receive her."The obstetrician said: it will be fine," recalls Linda Bloomstein."And Larry was by his side and I saw that he cried and moved his head in a sign of denial ... no".
At 2:00 am the neurosurgeon confirmed what the trauma specialist doctor had said four hours before: Lauren had Hellp syndrome.Then he gave worse news: his platelets (essential to stop the bleeding) were very low.But, according to Larry, the hospital did not have enough platelets there, so surgery should be postponed.Larry was baffled: how could it be that a regional medical center that brought babies to the world and performed all kinds of surgeries did not have hand platelets in case of an emergency.
Vaclavik called the Red Cross and other establishments, begging them to send what they had."In my understanding, there was a total lack of platelets in the state of New Jersey," he said in his statement.
They spent hours before the needy platelets arrived.
Neuro's team made a new scanner at 6:00 am.Larry did not dare to see him, "but for what they told me, it was much worse".While Lauren was in surgery, friends began to arrive seeing her and the baby, without realizing what had happened from the cheerful text messages of the previous night.At 12:30 pm, the neurosurgeon appeared and confirmed that the brain activity had stopped.Lauren was connected to a respirator without chance of recovering.
All this time, Hailey had been in the newborn area, being treated by the stunned colleagues in Lauren.They lowered her to Lauren's room and Larry put her in her mother's arms.After a few minutes, the nurses took the baby to the third floor to protect her from the germs.A respiratory therapist carefully removed the breathing tube from Lauren's mouth.At 3:08 pm, surrounded by their loved ones, he died.
En Estados Unidos, a diferencia de otros países desarrollados, las muertes maternas son tratadas como una tragedia privada y no como una catástrofe de salud públicacomo el de LaurenLauren's death was more public than usual.Hundreds of people attended their funeral, including hospital doctors and nurses, friends from all over the country, families that Lauren had attended.Vaclavik was there, devastated, Larry's family told.The head of the Monmouth Obstetrics Department presented his condolences and, according to Larry, during a private conversation promised to review what happened.
The days that followed Lauren's death, Larry could not assimilate the implications of what happened.He had to find a place to bury his wife, choose a coffin, write a tribute.He was too affected to return home in Mooresville, so he took Hailey to his parents' house, a room they rented while remodeling his house, and slept with the baby in the room during the first month.
After the funeral, he turned his attention to his daughter. No sabía nada de recién nacidos porque siempre pensó que Lauren le enseñaría."Nothing can be better than having a neonatal care nurse taking care of your baby," he had thought.He leaned on his mother and sister and Lauren's friends to learn.He took three months of work, but he barely approached the date of his return realized that he was not ready.“I don't think I can see a patient connected to a fan still.Or even a hospital bed, ”he warned.I didn't want to leave Hailey, so he resigned.
He sold the house, although he did not dare to deliver the keys."I couldn't give those keys to other people".He led Hailey a couple of times with his sister to Texas where he did not have to answer the constant questions.But traveling with his baby was hard.People didn't know what to think about him."People are not used to seeing a dad alone".Where I was going to feel that I was disconnected from everything."You go through this world and all these people are around you and continue with their lives and it is very, very insulating and you feel very alone".
Back to New Jersey, Larry found a job near his parents' house, did an operation and tried to resign.His employers convinced him to stay.To avoid reliving the funeral, he returned to Texas on the first anniversary of Lauren's death in September 2012.In one of his suitcases, he packed a giant cupcake mold that his wife had bought when they married.She thought it would be perfect for the first birthday cake they had.He cook the chocolate cake, Lauren's favorite, covered with sparks.
As Larry's paralysis vanished, his friends who were orthopedic began to press it.Larry doubted.Despite the mistakes he had witnessed, part of him wanted to believe that Lauren's death was inevitable. “Y mis amigos me decían: no podemos aceptar eso.With technology, every time a woman dies in childbirth, it is a medical error ".
Lauren's death was avoidable, he finally dared to admit Larry.He saw how the obstetrician and the nurses failed to recognize a typical case of pregnancy complications, not one, but several times over two days.For Larry, the fact that someone with the advantages that Lauren had died so unnecessarily, was a sign of a major problem.According to some standards, New Jersey has one of the highest maternal mortality rates in the United States.I wanted the authorities to reach the root of the problem: press the institutions to change.
That is the perspective of the United Kingdom, where maternal deaths are considered system failures.A national committee analyzes each death of a woman as a result of pregnancy or childbirth, and medical data and records are collected that help establish hospitals policies in the country.Forensics are even subject to public interrogations, which forces hospitals and their staff, to respond for their mistakes.This United Kingdom process is responsible for the amazing reduction of deaths from preeclampsia.The country's committee reported that it was a "success story" that they hope to repeat in other medical causes and conditions related to maternal death.
The United States does not have a comparable federal effort.Instead, the review of maternal mortality is at the discretion of the states.For this spring, 26 states (and the city of Philadelphia) had an established process, another five had committees with less than a year old.In almost every case, the resources are scarce, the reviews take years and the findings have little diffusion.A Bipartisan Law of the Congress, the 2017 maternal death prevention certificate would authorize financing to the States to establish reviews or improve their processes.
Relacionados
La mortalidad materna en EEUU: por qué las afroamericanas mueren cuatro veces más que las blancas
The New Jersey review team, the second oldest in the US, includes obstetricians, nurses, mental health specialists and even nutritionists.Using medical records and other reports, they identify each woman in the state who died up to a year after childbirth or pregnancy, for any reason, then they see their clinical chips and determine whether or not the cause was related to pregnancy.Every few years, the committee publishes a report that focuses on things such as the breed and age of mothers, the cause of death and other demographic data.In the past, these data have been used to promote policies that reduce postpartum depression.
But the New Jersey committee does not interview the relatives of the deceased person, nor analyze whether death was preventable.Like other states, "des-identifies" medical stories to eliminate any information that can point to a hospital or woman in particular.Otherwise, the medical community and legislators would refuse to do so.The goal is "to improve general care for patients," said Joseph Apuzzio, a professor of Obstetrics and Gynecology at the New Jersey Rutgers Medical Hospital, in charge of the Committee.This requires a process that is "prejudiced and non -punitive," he says."It is the best way to have a true discussion among all health providers that are present".
The result of this process, Larry concluded, is that the review is of little use to determine the responsibility for individual deaths or to assess whether some hospitals, doctors or nurses are more prone to error than others.For Larry this is a clear voluntary omission or denial.In a preventable death or other medical error, sometimes who and what are equally important as why: "unless someone is indicated specifically, I think the true cause of the problem will be lost," he says.
división de Licencias e InspecciónThey examined Lauren's card, interviewed their doctors and scrutinized Monmouth practices.In December 2012 they issued a report that corroborated everything Larry had seen firsthand."There is no record that the nurse notified the patient's high pressure doctor before childbirth," they concluded.And: "There is no evidence that blood pressure by the Obstetrician had been treated until the Code Stroke was issued".
El reporte culpó al hospital: “El centro no cumple los estándares de Nueva Jersey y falló en asegurarse de que el equipo siguiera las normas de obstetricia”.To respond to criticism, Monmouth implemented a corrective plan, also mentioned in the report.
The plan demanded an educational program on preeclampsia and Hellp syndrome, as well as critical care training in obstetrics for all nurses participating in childbirth, as well as more courses on the use of evidence -based methods to evaluate patients and forImprove communication between staff.
Some changes were basic: the nurses were trained in the need to review the prenatal history of the patient.They must now compare the blood pressure before and after childbirth and measure it every four hours at least.
An important part of the corrective plan involved Vaclavik, although neither the nurses were identified by name.The director of Obstetrics and Gynecology of the Monmouth gave "professional rehabilitation for the identified doctor", according to the report.There was also a "100% monitoring of doctors' records per month and every three months".This review focused on "compliance by the doctor for an intervention in time of the valuation and management of high pressure and pain".
The department leader, Robert Graebe, saw that Vaclavik's records complied with the standard in 100% of cases, according to Vaclavik himself during his deposition in the court.
When in March 2017 they asked Graebe if Vaclavik was exercising his functions in the hospital when treating Lauren, he replied: "He was and is".
In a separate note, the Health Department told Larry that he had forwarded his complaint to the Medical Council and the New Jersey Nurses Council.Neither of the two entities has taken disciplinary measures, according to their website.The copy of the Doh report came to Larry by mail.It was pleased by the findings but bewildered that they were not publicly revealed.No one would see them.
Months later, he sued Monmouth, Vaclavik and five nurses in the Supreme Court of Freehold, New Jersey.In order for a demand for medical malpractice to move forward in that state, an expert must certify that there are fundamentals.Larry's complaint was certified by a gynecologist obstetrician.But beyond the taking of statements, there has been no greater action around the case.
Inspired by the United Kingdom's model, the Maternal California Quality Care (CMQCC) nourishes the experiences of its founder, Elliott Main, Professor of Obstetry and Gynecology at Standford and the University of California-San Francisco, who for years led the departmentGynecology and Obstetrics of a San Francisco Hospital. “Uno de mis momentos más tristes como obstetra fue cuando una mujer con preeclampsia severa con la que pensamos haber procedido correctamente, todavía sufrió un ataque masivo y no pudimos salvarla”, dijo recientemente.That loss weighs him for 20 years.“When you have a maternal death you remember it for the rest of your life.All the details".
The CMQCC emerged a decade ago and seeks to reduce not only mortality, but also dangerous complications and racial disparities in obstetric care.It began by analyzing maternal deaths in the state over several years: in almost every case there was "at least some possibility of a better result".The most preventable deaths were those due to bleeding (70%) and preeclampsia (60%).
Main and his colleagues began to create a series of tools to help doctors and nurses to handle emergencies.The first, detecting the bleeding, recommends things such as: "Hellge cars" to store medications and supplies, protocols for mass transfusions and regular training and simulacros.Instead of the frequent examination of the "eye drop", which usually underestimate the importance of bleeding and delays treatment, nurses learned to collect and weigh the postpartum blood to have precise measures.
The hospitals that adopted this set of tools saw a decrease of 21% in deaths due to maternal bleeding in the first year.The hospitals that did not use this protocol had just a reduction of 1.two%.For 2013, according to Main, maternal deaths in California fell to 7 percent births, similar to the figures of Canada, France and Holland (a drastic cut of the trend in other parts of the US).
"Preventing is not a magical pill, it is actually a team job and it is vital to have a structured, organized and standardized approach in care," says Main.
The CMQCC tool kit to attend preeclampsia was launched in 2014 with emphasis on the type of protocols that could have saved Lauren: constant monitoring of blood pressure, aggressive and early treatment with hypertensive medications and magnesium sulfate.The data on its effectiveness have not been published.
This collaborative work inspired Vote and activists in several states to create their own initiatives.Much of the funds from 500 million to 10 years come from an initiative for maternal health funded by Merck, the pharmaceutical giant.It's called Merck for Mothers.
Originally it would go to less developed countries, but the company decided that it could not ignore the growing problem in the US.The mortality index is "unacceptable," says its executive director, Mary Ann etiebet. Hacer que el embarazo y el parto sean más seguros “no sólo salvará la vida de las mujeres, sino que mejorará nuestros sistemas de salud… para todos”.
Is just the beginning.According to the Institute of Medicine, it takes an average of 17 years for a new medical protocol to be adopted widely.Even in California, half of the 250 hospitals that bring babies to the world, still do not use the tools, warns Main, for whom the cause is inertia.
In the state of New York, some hospitals have questioned the need for what they call "Recipe of Medicine", says Mary D’Alton, from Columbia University.His answer: “Variability is the enemy of security.Instead of having ten different strategies for bleeding or hypertension treatment, choose one or two and make them consistent.When we do things in a standardized way, we have better results ".
A great lock: training.Other: money.Small suppliers, in particular, do not see the motivation to do so."It is difficult for a hospital to contribute the resources to change something that they do not see as a problem," says Bárbara Levy, of welcome.“If they have not had a maternal death because they only bring 500 babies to the world per year, how many years will they go until they see a severe problem?Ten "can pass".
In New Jersey, suppliers do not need much conviction thanks to a recent project to reduce blood loss in postpartum.The initiative comes from the Women's Health Association, neonatal and obstetric nurses.A large number of hospitals saw improvements.In one the average hemorrhages related to ICU went from 8 to 1.5 days.But only 31 of the 52 hospitals with State Obstetrics Units participate in the Plan, perhaps, because it is conducted by nurses, says Robyn D’Oria, director of the Central Jersey Family Health Consortium and a member of the State Maternal Mortality Committee."I remember talking to someone who thought progressistic in a hospital, and he said: I can't overcome what doctors do not want to participate in something like this".
So New Jersey hospitals will try again, this time adopting ‘Mini Kits’ for preeclampsia and hemorrhage, created by the Alliance for Maternal Health Innovation. “Is just the beginning” de algo que tomará al menos dos años, indica D’Oria.Among those who have contributed is Ryan Hansen, the teacher's husband who died months before Lauren in the same hospital.
The hospitals begin to act, while Mothers keep dying.One of them was Ashley Heaney Butler.Graduate from the University of Rutger, lived in Bayville where he decorated the walls of his house with anchors, because she was passionate about the ocean.He worked as a counselor at the New Jersey Vocational Rehabilitation Association.Her husband, Joseph, was a firefighter.
He gave birth to a healthy male in Monmouth in September last year and, a couple of weeks later, with just 31 years, he died without having left the hospital.He had an infection at the end of his pregnancy, possibly due to an anterior gastric bypass surgery.Was under the care of several doctors, including Vaclavik.
Jack Ennis felt Lauren's absence for the absence of calls.They were almost sisters and spoke several times a day.Sometimes Lauren called him to tell him that he was very tired and that they would speak later.He even called Ennis from Hawaii during his honeymoon.The night he died, Ennis knew that something was going wrong because he didn't know anything about her best friend."It took me for a long time that she wouldn't call me anymore, that affects me".
During Lauren's pregnancy, Frankie Hedges thought it would be like another Hailey grandmother.She and Lauren had many plans.Lauren's death implied the loss of his dreams for the extended family."I feel he didn't get what he deserved," Hedges said.
Vaclavik has an "greater" obstetric practice than in 2011 and continues to have privileges in Monmouth and two other hospitals."I will never forget Lauren's death, I will probably suffer from posttraumatic stress for this," he said in his testimony.
Hailey is 5 years old and the same brown hair and her mother's green eyes.He feels his mother's presence everywhere thanks to his dad and his new wife, Carolyn, with whom he married in 2014.They met at a hospital where Larry worked after Lauren's death.Lauren's photos and drawings are throughout the house in Holmdel, on the library shelves and up on the walls of the hallway.Larry and Carolyn spend free about Lauren and even Larry's youngest daughter, Aria, 2 years old, calls her "Mama Lauren".
On birthdays and parties, Larry takes girls to the cemetery.He designed the tombst.Larry has done what he can to keep the family together.Ennis and Hedges and their families participate in each important celebration.
Larry still has Lauren's video and Hailey on his phone."From far the hardest thing to accept is what happened, from Lauren's perspective".Looking at the clip on a recent night, and seeing it alive again, he thought: “I can't, I can't accept it.The amount of pain that you have had to experiment at that time when she finally had this baby ... I can accept my pain, ”he says while he sees Lauren stroking Hailey's cheek."But your pain is something I can't accept.I can not understand.I can't unravel it ".
Do you know someone who died or almost died during childbirth?Please tell us your story in this form.You can also write to maternal@propublica.org.Derek Kravitz and Adriana Gallardo de Propublica and Bo Erickson of NPR contributed to this research and reported for this story.Spanish translation: Carmen Méndez, María Isabel Capiello and Eulimar Núñez.Photos: Bryan Anselm for Propublic.
ComparteRELACIONADOS:Embarazo•Salud y Mujer•Muertes•Procedimientos Médicos•








